Our immune system works to protect our body against infection, illness and disease. It also works to protect us from the development of cancer. The immune system includes the lymph glands, spleen and white blood cells.
The immune system fails to recognise cancer cells
The cancer cells produce signals that stop the immune system from attacking it
The cancer cells hide or escape from the immune system
Cancer can weaken the immune system
Cancer treatments might weaken the immune system
The immune system may help to fight cancer
Chemotherapy
Radiotherapy
High dose of steroids
Immunotherapy is modern science that uses our immune system to fight cancer. It works by helping the immune
system recognise and attack cancer cells. It is a major breakthrough in the field of science and modern medicine in
treating cancer. For a very long time, we have been treating cancer by either burning it through radiation, cutting or
removing it by surgery or poisoning the cancer cells with chemotherapy. This has resulted in lesser cures and
numerous, unwanted side effects. So now, there's a new and different approach to treat cancer- one that acts on the
patient's immune system, instead of cancer.
Immunotherapy leads the way forward to finding better cures as well as reducing the adverse effects.
Immunotherapy is a more personalised and tailor-made approach to cancer, as opposed to treating cancer by a "one-size-fits-all" approach. It also happens to be a more targeted treatment, bringing minimal to no collateral damage to
the body.
Immunotherapy is an umbrella term that encompasses different modalities to boost the immune system to fight
cancer. Some of these are also called Biological therapy or Targeted therapy.

Monoclonal antibodies (MABs) recognise and attack certain proteins on the surface of cancer cells

Vaccines
help the immune system to recognise and attack cancer

Cytokines are a group of proteins, naturally found in the body. They help to boost the immune system.

CAR T-cell therapy (also called adoptive cell transfer) to change the genes in a person's white blood cells .

Checkpoint inhibitors are a type of immunotherapy that block different checkpoint proteins.
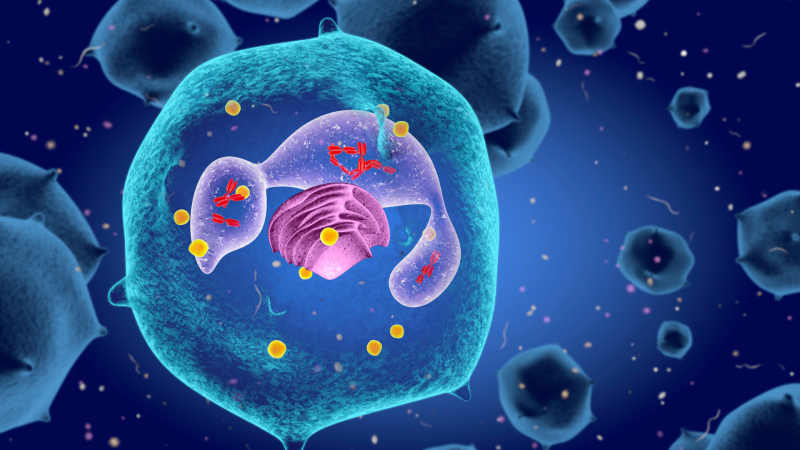
Traditionally, we have been treating cancer by attacking it with chemotherapy, radiation, or by removing it with surgery. The "cut, burn and poison" techniques are estimated to treat half of the cases diagnosed with cancer, but what about the other half? For a very long time, physicians have been trying to kill mutating versions of our own cells, trying to kill the bad ones, sparing the good ones, and making ourselves sick in the process. But now there's a new and effective approach to treat cancer- one that acts on the patient's immune system, instead of cancer. Our immune system is the most effective natural defence against disease. Anything that's not supposed to be in the body, gets destroyed by the immune system. Cells of the immune system are on constant patrol to attack and destroy any invaders that make us sick, including cells that mutate to develop into cancer.
The immune cells such as T cells and
Dendritic cells (the key antigen-presenting
cells) defend and protect the body.
The Dendritic cells patrol the body looking
for cancer cells and other organisms
causing diseases. (They act as informer
cells). The T cells, on the other hand, are the
soldiers of the immune system that actually
do the cancer-killing process.
When the Dendritic cell finds a suspicious
cell, it sends a specific signal to the T cell to
multiply and attack the suspicious cell.
That's how the cancer-killing process takes
place.
The answer is, it does try to kill cancer, but cancer evades the immune responses. In other words, cancer escapes or hides from the immune system shuts down the defences and avoids the fight.
Cancer immunotherapy is an approach to defeat cancer, by unmasking cancer, unleashing the power of the immune system and starting the fight, again. Cancer immunotherapy is often understood as a recent discovery when in actuality it dates back to antiquity. Despite its long history, it has blossomed into fruition only in recent years with the advances of multiple forms of treatment, including cancer vaccines, adoptive cell transfer, chimeric antigen (CAR) T cell, and immune checkpoint inhibitors. The good part is that our immune system has an amazing capacity for remembering disease-causing agents so immunotherapy promises a unique opportunity to treat cancer successfully and achieve prolonged remission.
Yes, we can make cells/ substances in the lab, just like immune cells/components, and use them to HELP our immune system fight cancer cells.
This is done by making substances in a lab that are just like immune system components and using them to
help restore or improve how your immune system works to find and attack cancer cells
The other way is to modify or train cells to become cancer-fighting cells. These cells when given back to the
body jumpstart the process of killing cancer

Smoking leads to mutations in our DNA. In other words, it means that the DNA gets damaged, due to tobacco smoking. This damaged or mutated DNA, in turn, gives rise to abnormal protein in our lung cells. Proteins that are changed or abnormal, stop functioning normally. This makes the cell become defective (cancerous) and grows and divides uncontrollably to form cancer. The mutated proteins are broken down into small pieces and presented on the surface of cancer cells. These abnormal peptides are recognised as foreign and activate the T cells to kill the cancer cells.
Sometimes, the immune system fails to do its job. The immune response against cancer may not be strong enough or cancer cells may evade the immune responses. Cancer develops ways to escape immune- recognition. When this happens, the immune system is unable to mount an attack on cancer cells, in turn giving rise to more cancer cells growing bigger and stronger. With this weakened immune system, cancer gets a chance to grow and metastasise, what is called stage 4 cancer. The cancer spreads to other parts of the body making it difficult to treat
Cancer is best treated by a multi-modal approach. A multi-modal approach is a comprehensive approach that includes surgery, radiation, chemotherapy as well as immunotherapy. It also includes alternative and complementary systems of medicine. Cancer is a difficult-to-treat disease, hence a comprehensive approach is the best way to treat it. Cancer and its treatment both bring a lot of suffering to the patient. It is not enough to treat a patient with conventional methods alone, without treating the pain, fatigue, the depression that comes with it. A cancer patient needs a complete treatment plan to get rid of cancer and the associated problems.
Several studies are showing that Immunotherapy has the power to "cure" cancer, a word used with caution by Oncologists. The immune system once activated against cancer, not only kills cancer but also memorises the event of killing. Thus when cancer arises again, the immune system mounts an attack against it, in the same way, it did the first time, killing the recurrent cancer cells and bringing about a cure in cancer. Unless we give the immune system a chance to eradicate cancer, we can not be sure of complete recovery or cure.

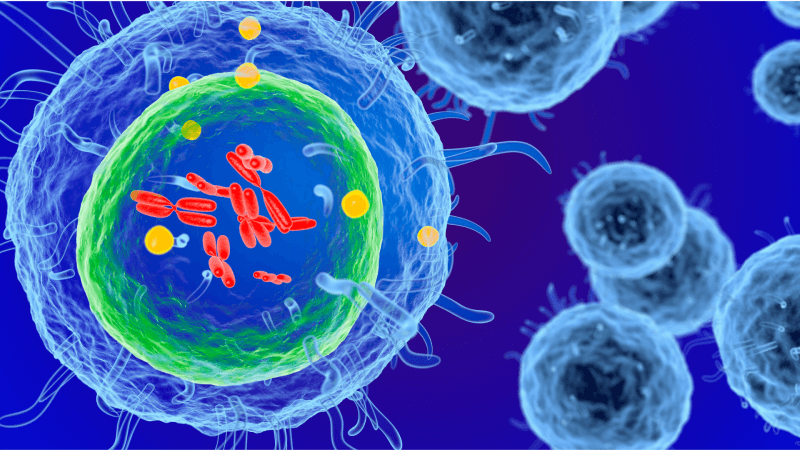
Immunotherapy is often perceived as a relatively recent advance when in reality it is an ancient science. From ancient Egypt, some 3000 years ago, to the early 19th century there have been multiple reports of tumours disappearing spontaneously or after an infection with a high fever. The similarity between cancer and inflammation were described for the first time by the Greek physician Galen, who observed that cancer might evolve from inflammatory lesions. The most significant advances came from William B. Coley who is known as the Father of Immunotherapy. He observed a number of cases in which potentially incurable cancer patients went into spontaneous remission after developing an acute bacterial infection. Despite the success, the lack of mechanism of action for Coley's methods as well as the risk of infecting cancer patients caused oncologists to prefer surgery and radiotherapy and Coley's legacy was widely forgotten and dismissed for some decades
Interest in the immune system came up again after 1945, with the discovery of interferon and the very first
cancer vaccine. The existence of T cells and their very crucial role in immunity was discovered in the late
1960s by Jacques Miller, followed by the discovery of Dendritic cells by Ralph Steinman in 1973, and
natural killer (NK) cells in 1975 by Klein, which paved the way forward. Finally in the 1980s, when the
vaccine against hepatitis B was discovered, the field of immunotherapy emerged and optimism resurfaced
that immunotherapy might be used to treat many diseases including cancer and propelled research into
where we are at the moment.
Around 50 years ago, professor Lloyd J Old, pioneer of cancer immuno-oncology correctly predicted that
in the future immunotherapy would be the 4th kind of cancer therapy., and immunotherapy has rightly
claimed as the legitimate 4th pillar of cancer treatment after surgery, radiation and chemotherapy.
Numerous contributions have been made in this field, and this field is growing at a rapid pace as it shows
promising responses in a large number of patients, worldwide.
Dendritic cells are the most
special cells, and the most
efficient cells of the
immune system, that have
the power to initiate the
process of cancer-killing
Dendritic cells (DC) are the most specialised cells of the immune system. They are also the
most efficient as they can capture the most insignificant amount of antigens and break them
into peptides to activate T cells. They are the only cells of the immune system that can
initiate antigen-specific immune responses.
Dendritic cells have finger-like projections, that capture their targets like bacteria, viruses
or cancer cells. At first, they internalize it, then break it down to peptides, and then project
the peptides on their surface, for T cells to recognise them. When a naive T cell comes in
close proximity to a Dendritic cell, there is stimulation of the T cell. The naive T cell gets
converted to a committed T cell- i.e. committed to doing its job of killing the target enemy.
This is how the infections are fought, as well as how the cancer cells are killed by the
immune system.
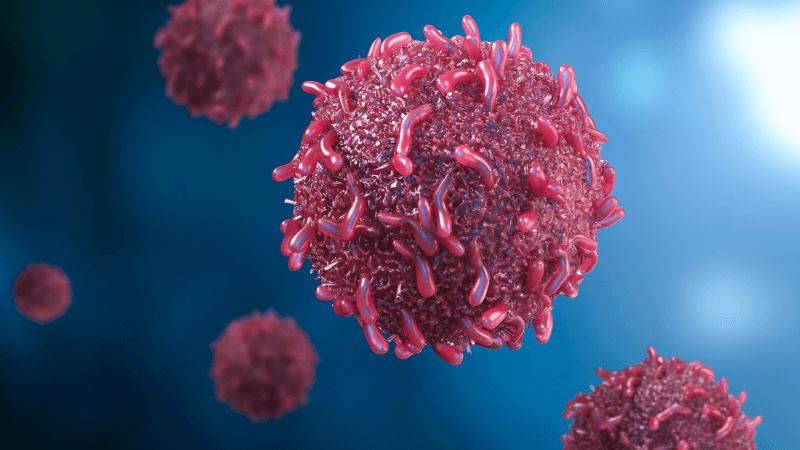

-that works to boost immunity against cancer
Dendritic cells are cells of the immune system that help in the fight against cancer.
Denvax is your personalised cancer treatment that involves cancer-fighting dendritic cells. Being
autologous, it is non-toxic and does not interfere with an ongoing treatment plan or the patient’s daily
routine.
Denvax is a treatment for most solid tumours, including lymphoma and multiple myeloma. It can be given
at any stage of the disease. It is targeted therapy and comes under the 4th modality of cancer treatment
called cancer Immunotherapy. The other three are Surgery, Radiation and Chemotherapy.
In cancer, the immune system fails as cells of the immune system fail to recognise the cancer cells. The immune system doesn’t “see” tumours as foreign or dangerous, and doesn’t mount a strong attack against them. Another reason tumours may not stimulate an immune response is that cancer cells develop ways to escape the immune system. A dendritic cell is a specialised cell that boosts immune responses in our body, by correcting the failure to recognise the cancer cell. The activated immune system then circulates throughout the body and destroys the cancer cells.
Denvax is an Adjuvant/Additional treatment plan. It helps to fight cancer by killing the cancer cells. It works
by activating the immune system against cancer. Cancer is best treated by a multi-disciplinary approach. The
other treatment modalities including surgery, radiation and chemotherapy also help to kill the cancer cells.
Denvax adds to this arsenal of killing cancer. It helps to improve quality of life, prolong life and give
better clinical outcomes.
Denvax has little or no conflict with other treatment modalities. Being autologous (self), it is almost non-toxic and does not interfere with the patient’s ongoing treatment plan or his/her daily routine. In stage IV
patients, it works as palliative therapy, which helps in giving comfort to the patient.
In this technique, the patient’s own blood cells are taken and transformed into dendritic cells that are
trained to fight cancer cells. These dendritic cells given back to the patient initiate a fight against the disease
at the cellular level and help in stopping cancer.
The first dose manufactured is given to the patient on the 10th day of blood collection. Subsequent doses are
administered at 2- weeks intervals.
To begin Denvax treatment, the patient or the attendant is required to contact our office, preferably nearby
the patient's location. The patient is then required to send his reports and a short video, explaining or showing
his/her current clinical status.
The doctor evaluates the patient's clinical condition and may or may not advise Denvax, based on Eligibility
Criteria. Patients willing to take Denvax treatment are required to fill and sign an Informed Consent Form. The
logistics team then works on the collection of blood drawn from the patient’s home. They assign a trained
technical staff to travel to the patient’s location for blood collection.
It takes 8 days to manufacture Denvax. The patient may choose to get the Denvax dose in the comforts of their
home or visit any of the Denvax clinics for receiving the dose. Trained technical staff along with Denvax dose is
sent to the patient's home for administration. The technical staff leaves the patient's home only after the dose
is safely received by the patient. Further doses are administered the same way.
Denvax has negligible adverse effects or toxicity as compared to chemotherapy. Being an autologous treatment it is safe and has minimal side effects. Some patients may experience fever for a day or two after taking Denvax therapy.


}})
Cancer is rising to epidemic proportions. Unless we change the rules of treating cancer, we cannot make progress in bringing cures. Cancer prevention is one way of reducing the suffering and mortality in this disease. The other way is early diagnosis along with a comprehensive treatment plan.
or a very long time, we have seen patients struggle with cancer. We also know cancer needs a different approach in order to find respite, and that we need to move fast. Thankfully, Immunotherapy has come up in a big way, bringing not just hope but also cures in this disease. We are fortunate to have pioneered this work in India when the word "Immunotherapy" was almost unheard of. We hope to create history by bringing the best possible treatment in cancer, that is not just safe, but also affordable and easy to access in all parts of our country. We are thankful to our patients who have put so much trust in us and given us a chance to prove the worthiness of this treatment. Here's wishing everyone health and happiness!
“We have the largest experience of 18+ years in treating various cancers using Dendritic cells. From our clinical experience, we find that Denvax helps most cancer patients in varying degrees. The majority of the patients respond favourably in some form or the other, A minority may show no response at all, whereas a small group may even enter into a cure. At, The Denvax Clinics, we keep making endeavours and progress to better the clinical outcomes and help our patients achieve long and disease-free life."


