Immunotherapy For Pancreatic Cancer
Pancreatic cancer stands as one of the most aggressive and deadliest forms of cancer, with a hauntingly low survival rate. Traditional treatment options, such as surgery, chemotherapy, and radiation therapy, often yield limited success due to the cancer’s propensity for rapid spread and resistance to conventional therapies. However, amidst the challenges posed by this formidable disease, a beacon of hope emerges in the form of immunotherapy—a groundbreaking approach that holds the potential to revolutionize the treatment landscape for pancreatic cancer patients.
Understanding Pancreatic Cancer
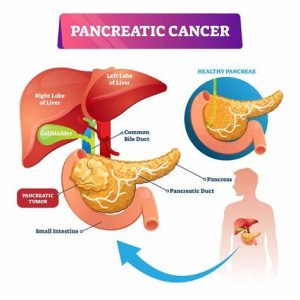
Pancreatic cancer arises when malignant cells form in the tissues of the pancreas, an essential organ responsible for producing digestive enzymes and hormones, including insulin. Due to its location deep within the abdomen and lack of early symptoms, pancreatic cancer is frequently diagnosed at an advanced stage, making it notoriously difficult to treat. Moreover, the aggressive nature of pancreatic cancer and its tendency to metastasize further complicate treatment efforts, necessitating novel therapeutic strategies to improve outcomes.
The Promise of Immunotherapy
Immunotherapy represents a paradigm shift in cancer treatment, leveraging the body’s own immune system to recognize, target, and destroy cancer cells. Unlike traditional treatments that directly attack tumors, immunotherapy enhances the immune response, enabling it to more effectively identify and eliminate cancerous cells while sparing healthy tissue. This approach offers several potential advantages in the context of pancreatic cancer:
- Targeted Precision: Immunotherapy drugs, including checkpoint inhibitors and adoptive cell therapies, specifically target cancer cells while minimizing damage to surrounding tissues, thereby reducing side effects and improving treatment tolerability.
- Overcoming Resistance: Pancreatic cancer is notorious for its resistance to chemotherapy and radiation therapy. Immunotherapy offers a complementary approach that may overcome resistance mechanisms, providing a viable treatment option for patients who have failed conventional therapies.
- Personalized Treatment: Immunotherapy can be tailored to the individual patient’s immune profile, allowing for a more personalized and targeted approach to treatment. Biomarkers such as tumor mutational burden (TMB) and microsatellite instability (MSI) can help identify patients who are most likely to benefit from immunotherapy.
- Combination Therapies: Immunotherapy can be combined with other treatment modalities, such as chemotherapy, targeted therapy, or radiation therapy, to enhance efficacy and improve outcomes. These combination approaches have shown promise in clinical trials and real-world studies, offering new avenues for treatment optimization.
Evidence of Effectiveness
While the efficacy of immunotherapy in pancreatic cancer is still being explored, recent studies have yielded encouraging results, highlighting its potential as a valuable addition to the treatment arsenal.
- Improved Survival Rates: Clinical trials evaluating checkpoint inhibitors in patients with advanced pancreatic cancer have shown promising improvements in overall survival compared to standard chemotherapy alone. These findings offer hope for patients who previously had limited treatment options.
- Disease Control: Immunotherapy has demonstrated the ability to control disease progression in some patients with pancreatic cancer, leading to tumor stabilization or regression and delaying the need for further treatment interventions.
- Enhanced Quality of Life: By reducing symptoms associated with advanced pancreatic cancer, such as pain, nausea, and fatigue, immunotherapy can significantly enhance patients’ overall quality of life, allowing them to better cope with the physical and emotional toll of the disease.
Challenges
Despite its considerable promise, immunotherapy faces several challenges in the treatment of pancreatic cancer, including:
1. Tumor Microenvironment: Pancreatic tumors create an immunosuppressive microenvironment that inhibits immune cell function and promotes tumor growth. Overcoming these immunosuppressive barriers remains a significant challenge in optimizing the efficacy of immunotherapy for pancreatic cancer.
2. Biomarker Identification: Identifying predictive biomarkers that can accurately predict response to immunotherapy is essential for selecting the most appropriate patients and optimizing treatment outcomes. Current biomarkers, such as PD-L1 expression and TMB, have shown promise but may not fully capture the complexity of immune responses in pancreatic cancer.
3. Combination Strategies: Developing optimal combination strategies that synergize with immunotherapy to enhance efficacy and overcome resistance mechanisms is an area of active research. Clinical trials evaluating novel combination regimens are underway to address this need.
Final Note
In the battle against pancreatic cancer, immunotherapy offers a glimmer of hope for patients and clinicians alike, heralding a new era of personalized and targeted treatment approaches. While challenges remain, the promise of immunotherapy in pancreatic cancer holds the potential to transform outcomes and improve quality of life for individuals facing this devastating disease. As research continues to advance and our understanding of the complex interplay between the immune system and cancer grows, the future of immunotherapy in pancreatic cancer looks increasingly promising, offering renewed optimism for patients and caregivers alike.
Also Read: What is the Success Rate of Immunotherapy?







