

For decades, the Oncology community are trying to understand the role of obesity in cancer risk and its outcomes. It is estimated that a fifth of the world, almost 640 million people are obese. Obesity is the disproportionate body weight for height. It is expressed in terms of BMI (body mass Index). A BMI of more than 30 is considered obesity. Below are some of the important findings:

Obesity is found to be strongly associated with developing and dying from several major illnesses, including heart disease, type 2 diabetes and cancer.

It is quickly overtaking smoking as the preventable cause of cancer. Some 20% of new cases, and 17% of cancer-related deaths are attributable to obesity.

Interesting to note is that, majority of adults remain unaware of the relationship between obesity and cancer.

A landmark study of 9 lacs individuals, showed that obese people were upto 50-60% more likely to develop and die from cancer, compared to their normal counterparts.

Researches are showing losing weight can help reduce co-morbidities, cancer risk, and early death. Let's learn more about obesity.
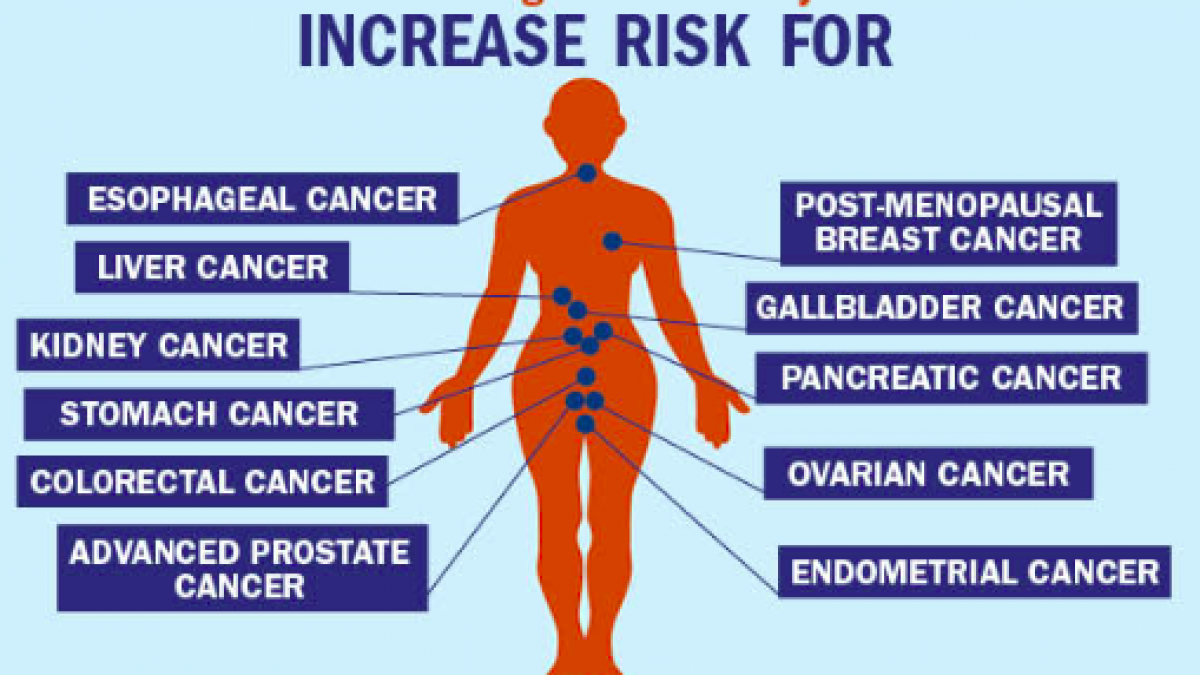
"Obesity is, in itself, a state of chronic inflammation."
Obese people have presence of low-levels of chronic inflammation, which can over time,
cause DNA damage and lead to cancer. Overweight and obese individuals are more likely to
have conditions linked with chronic inflammation that are risk factors for cancer. For
example, obesity, is linked with diabetes, which is a low level chronic inflammatory state that
also promotes cancer formation. Another example is chronic inflammation induced by
gastroesophageal reflux disease (GERD), or Barrett esophagus, a likely cause of esophageal
cancer. Obesity is a risk factor for gallstones, which is a strong risk factor for gallbladder
cancer.
The other mechanism that works in promoting cancer in obese people is through production
of excess levels of estrogen in fatty tissues, also called as adipose tissue. This increases risk of
breast cancer, endometrial cancer, ovarian cancer and other cancers.
Obese people also have increased levels of insulin and insulin-like growth factors. When these
factors are found in increased amounts in the blood, it leads to a condition called
hyperinsulinemia, or insulin resistance, and this precedes the development of type 2
diabetes. These 2 factors, ie insulin and IGF-1 promote the development of colon cancer,
kidney cancer, prostate cancer, and endometrial cancers.

Obesity Changes both Cancer and its treatment outcomes
Research indicates that obesity may
worsen several aspects of cancer
survivorship, including quality of life,
cancer recurrence, cancer progression, and
prognosis.
For example, obesity is associated with
increased risks of treatment-related
lymphedema in breast cancer survivors
and incontinence in prostate cancer
survivors treated with radical
prostatectomy. It may also be linked to an
increased risk of recurrence.
It is the excess fat (extra-abdominal
adiposity) and low muscle at the time of
diagnosis that may be associated with
poor treatment outcomes. Obesity
influences treatment tolerance. There are
more treatment-related complications, like
poorer wound healing after surgery.

There is sufficient evidence to state that obesity is linked with increased risk of developing 13- different cancer types. The strongest association is with endometrium (uterine) cancer in females. The list includes oesophageal cancer, stomach cancer, liver, kidney, breast, colorectal, prostate cancer among others. Another important finding is that individuals who are obese at the time of diagnosis, have increased risk of recurrence and mortality compared to normal weight counterparts. There is consistent evidence that higher amounts of body fat are associated with increased risks of a number of cancers including:
Obese and overweight women are two to about four times as likely as normal-weight women to develop endometrial cancer (cancer of the lining of the uterus), and extremely obese women are about seven times as likely to develop the more common of the two main types of this cancer. The risk of endometrial cancer increases with increasing weight gain in adulthood, particularly among women who have never used menopausal hormone therapy.
People who are overweight or obese are about twice as likely as normal-weight people to develop a type of esophageal cancer called esophageal adenocarcinoma, and people who are extremely obese are more than four times as likely.
People who are obese are nearly twice as likely as normal-weight people to develop cancer in the upper part of the stomach, that is, the part that is closest to the esophagus.
People who are overweight or obese are up to twice as likely as normal-weight people to develop liver cancer. The association between overweight/obesity and liver cancer is stronger in men than women.
People who are overweight or obese are nearly twice as likely as normal-weight people to develop renal cell cancer, the most common form of kidney cancer. The association of renal cell cancer with obesity is independent of its association with high blood pressure, a known risk factor for kidney cancer.
Compared with normal-weight individuals, overweight and obese individuals have a slight (10% to 20%) increase in the risk of developing multiple myeloma.
The risk of this slow-growing brain tumor that arises in the membranes surrounding the brain and the spinal cord is increased by about 50% in people who are obese and about 20% in people who are overweight.
People who are overweight or obese are about 1.5 times as likely to develop pancreatic cancer as normal-weight people.
People who are obese are slightly (about 30%) more likely to develop colorectal cancer than normal-weight people. A higher BMI is associated with increased risks of colon and rectal cancers in both men and in women, but the increases are higher in men than in women.
Compared with normal-weight people, people who are overweight have a slight (about 20%) increase in risk of gallbladder cancer, and people who are obese have a 60% increase in risk of gallbladder cancer. The risk increase is greater in women than men.
Among postmenopausal women, those who are obese have a 20% to 40% increase in risk of developing breast cancer compared with normal-weight women. The higher risks are seen mainly in women who have never used menopausal hormone therapy and for tumors that express hormone receptors. Obesity is also a risk factor for breast cancer in men. In premenopausal women, by contrast, overweight and obesity have been found to be associated with a 20% decreased risk of breast tumors that express hormone receptors.
Higher BMI is associated with a slight increase in the risk of ovarian cancer, particularly in women who have never used menopausal hormone therapy (24). For example, a 5-unit increase in BMI is associated with a 10% increase in risk among women who have never used menopausal hormone therapy.
Higher BMI (specifically, a 5-unit increase in BMI) is associated with a slight (10%) increase in the risk of thyroid cancer.
A large percentage of cancers in young adults are due to poor dietary intake and being overweight and obese.
Excess body weight could account up to 60% of all endometrial cancers, 36% of gallbladder cancers, 33% of
kidney cancers, 17% of pancreatic cancers, and 11% of multiple myeloma.
Childhood and adolescent obesity are found to have increased risk of colorectal, endometrial, and pancreatic
cancers with multiple myeloma.
Having diabetes, gallstones, inflammatory bowel disease, and poor diet in young adults contribute to getting
cancer at early age.
Poor dietary habits like low intake of fruits and vegetables, and high intake of red meat and processed meats
are contributing to increased rates of cancers, worldwide. Low intake of fish, whole grains and high
consumption of sodium and sugar sweetened beverages are all contributory to greater incidence of cancer.
BMI is a useful tool to assess obesity or being overweight. Majority of physicians do not assess a patient's BMI, and majority do not diagnose obesity or advise their patients on losing weight.
Children and young adults need to be screened periodically for obesity and related health issues. Urban planning for promoting physical activity, regulation on sugar-sweetened beverages, and restriction on their advertising is required as additional measures to stop the obesity epidemic.


Avoiding weight gain or losing weight decreases the risk of Cancer
Many studies have provided consistent evidence that people who have lower weight gain
during adulthood have lower risks of colon cancer, kidney cancer, and—for postmenopausal
women—breast, endometrial, and ovarian cancers.
Studies have also shown possible associations between weight loss and cancer risk. Some of
these have found decreased risks of breast, endometrial, colon, and prostate cancers among
people who have lost weight.
Stronger evidence for a relationship between weight loss and cancer risk comes from studies
of people who have undergone bariatric surgery (surgery performed on the stomach or
intestines to induce weight loss). Obese people who have bariatric surgery
appear to have
lower risks of obesity-related cancers than obese people who do not have bariatric surgery
A significant finding showed patients who underwent bariatric surgery for losing weight,
showed lesser breast and endometrium cancer rates. Encouraging weight loss in patients, can
help reduce co-morbidities, cancer risk, as well as early death.
}})
Cancer is rising to epidemic proportions. Unless we change the rules of treating cancer, we cannot make progress in bringing cures. Cancer prevention is one way of reducing the suffering and mortality in this disease. The other way is early diagnosis along with a comprehensive treatment plan.
or a very long time, we have seen patients struggle with cancer. We also know cancer needs a different approach in order to find respite, and that we need to move fast. Thankfully, Immunotherapy has come up in a big way, bringing not just hope but also cures in this disease. We are fortunate to have pioneered this work in India when the word "Immunotherapy" was almost unheard of. We hope to create history by bringing the best possible treatment in cancer, that is not just safe, but also affordable and easy to access in all parts of our country. We are thankful to our patients who have put so much trust in us and given us a chance to prove the worthiness of this treatment. Here's wishing everyone health and happiness!
“We have the largest experience of 18+ years in treating various cancers using Dendritic cells. From our clinical experience, we find that Denvax helps most cancer patients in varying degrees. The majority of the patients respond favourably in some form or the other, A minority may show no response at all, whereas a small group may even enter into a cure. At, The Denvax Clinics, we keep making endeavours and progress to better the clinical outcomes and help our patients achieve long and disease-free life."


